Our story so far, and what’s next for Plum
Circa 2019 – Saurabh and I are speaking to maybe our 100th CHRO to understand their world and figure what Plum can really help them solve. We get lots of inputs, metrics, and jargon – Coverage, Network, Copay, etc - but we keep hearing, between the lines, about the moment of impact.
The claim.
What an employee goes through in their most vulnerable moment. We knew then, and we believe now, that the claims experience is the most important thing when it comes to insurance. Corporate or Personal. Almost everybody we knew (and then some) had a story around their insurance claim, and almost nobody had nice things to say about it. This hunch was further validated when the pandemic hit.
In that moment, we realised, and decided that impact could only come from building the best claims experience in the world.
We've been obsessing over this for the past 6 years. Perhaps more than anyone else in the world. And we know today that we were right to do so.
After six years of investments, both incremental and impactful, we can say that Plum’s claims experience is the best in the world.
How do we know? We have the highest NPS in the business.
NPS is an extremely difficult metric to crack. For context, the biggest e-commerce brand scores close to 50, and the gold standard in service scores a tad over 60. We measure NPS for claims, which makes it all the more challenging – most companies don't even measure it.
We are incredibly proud of our NPS which stands at an industry-leading 79. What makes it better is that we’ve stayed on this score despite scaling 60x in the number of claims processed.
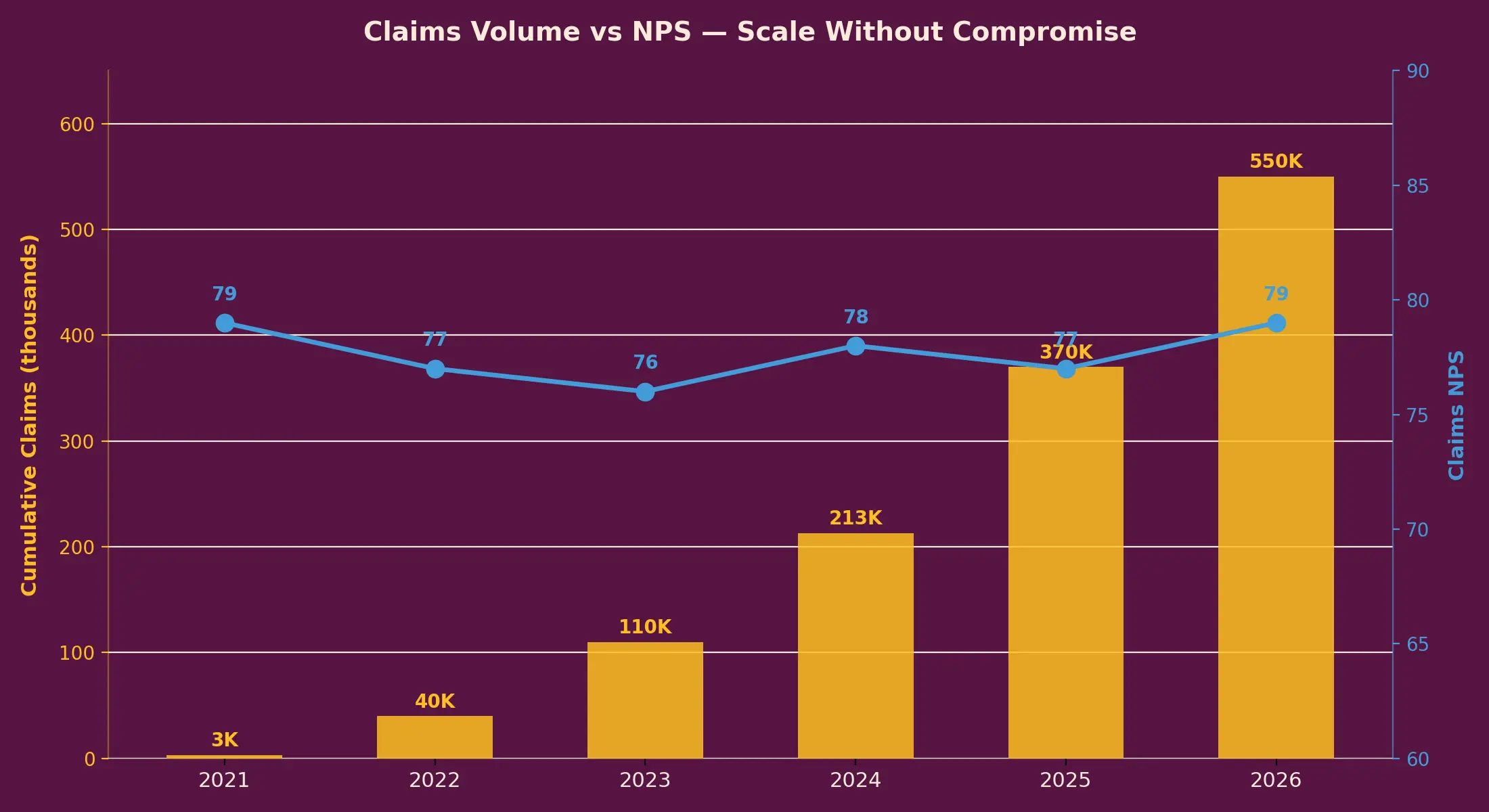
What we focused on to get here.
Our NPS is a result of every team working in tandem to influence every touch point of the claims experience, across four foundational principles – speed, seamlessness, value, and ease.
Speed
Our cashless claims experience is so fast that you can start booking your Uber immediately after your doctor okays your discharge. The median reimbursement claim on Plum gets resolved in hours. Not days, weeks, and certainly not months.
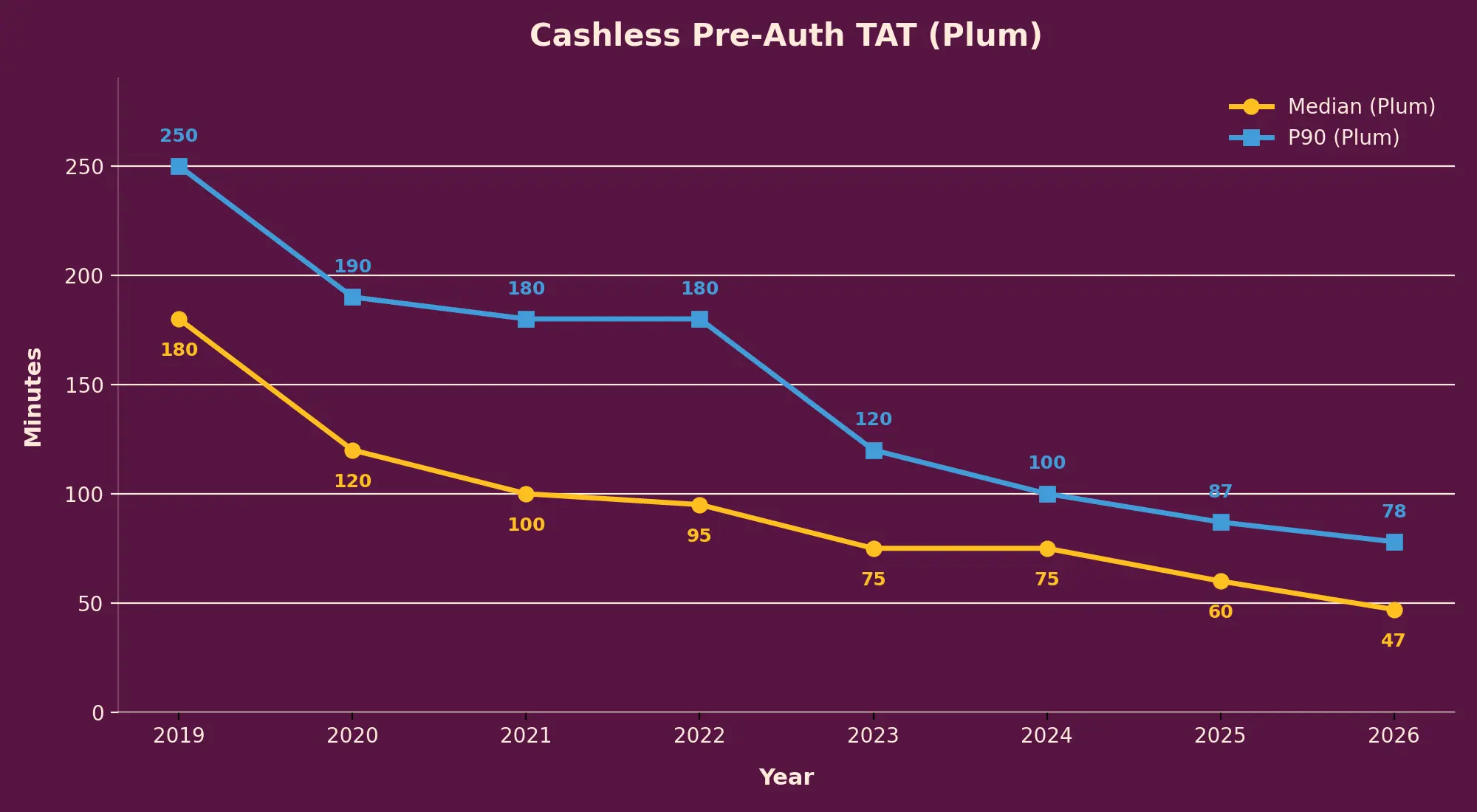
The industry benchmark today for median and P90 is 90 minutes and 120 minutes, respectively.
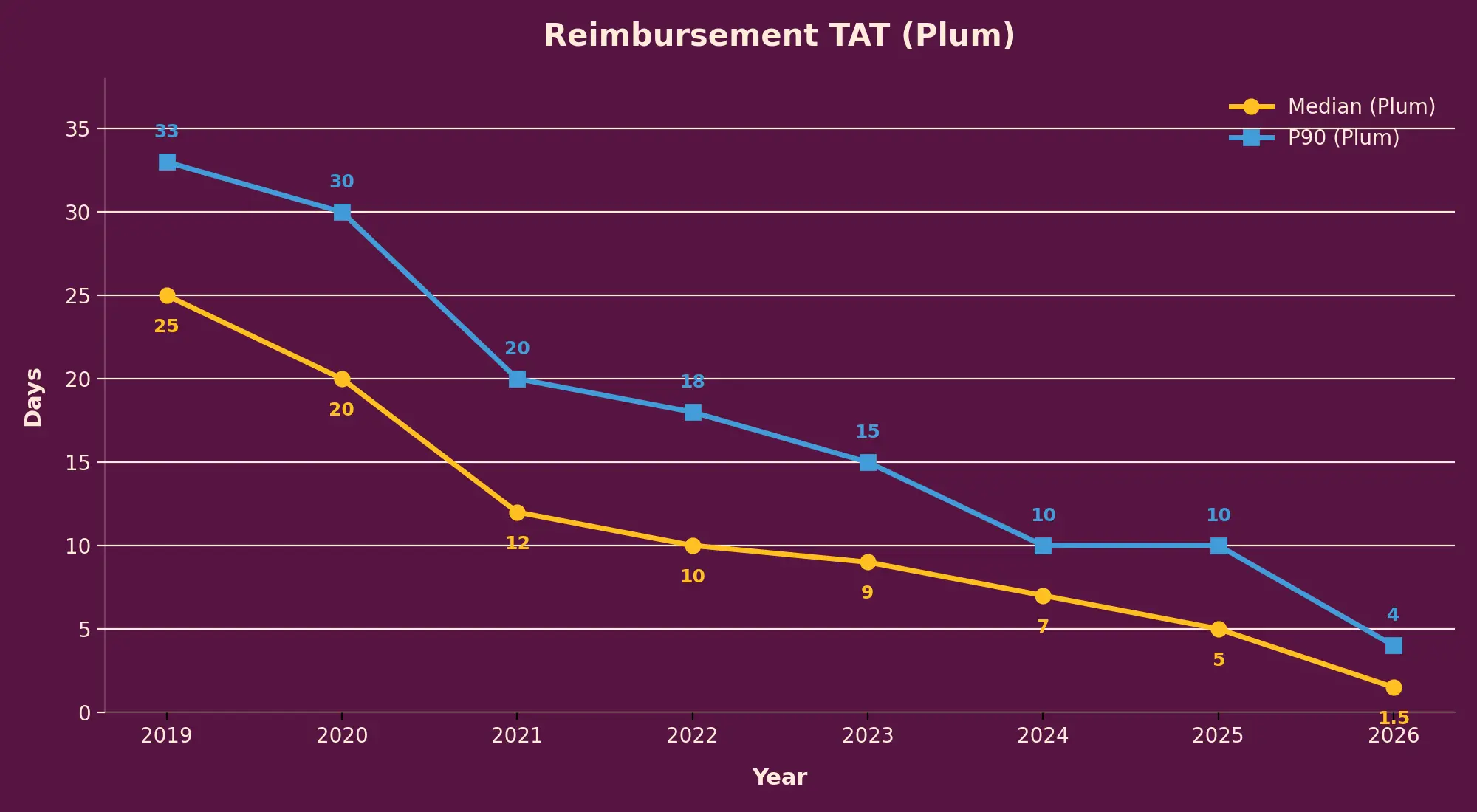
The industry benchmark today for median and P90 is 12 days and 24 days, respectively.
Seamlessness
Today, 78% of our claims go through without having to speak to a human in the loop – all you had to do was raise the claim on the Plum app.
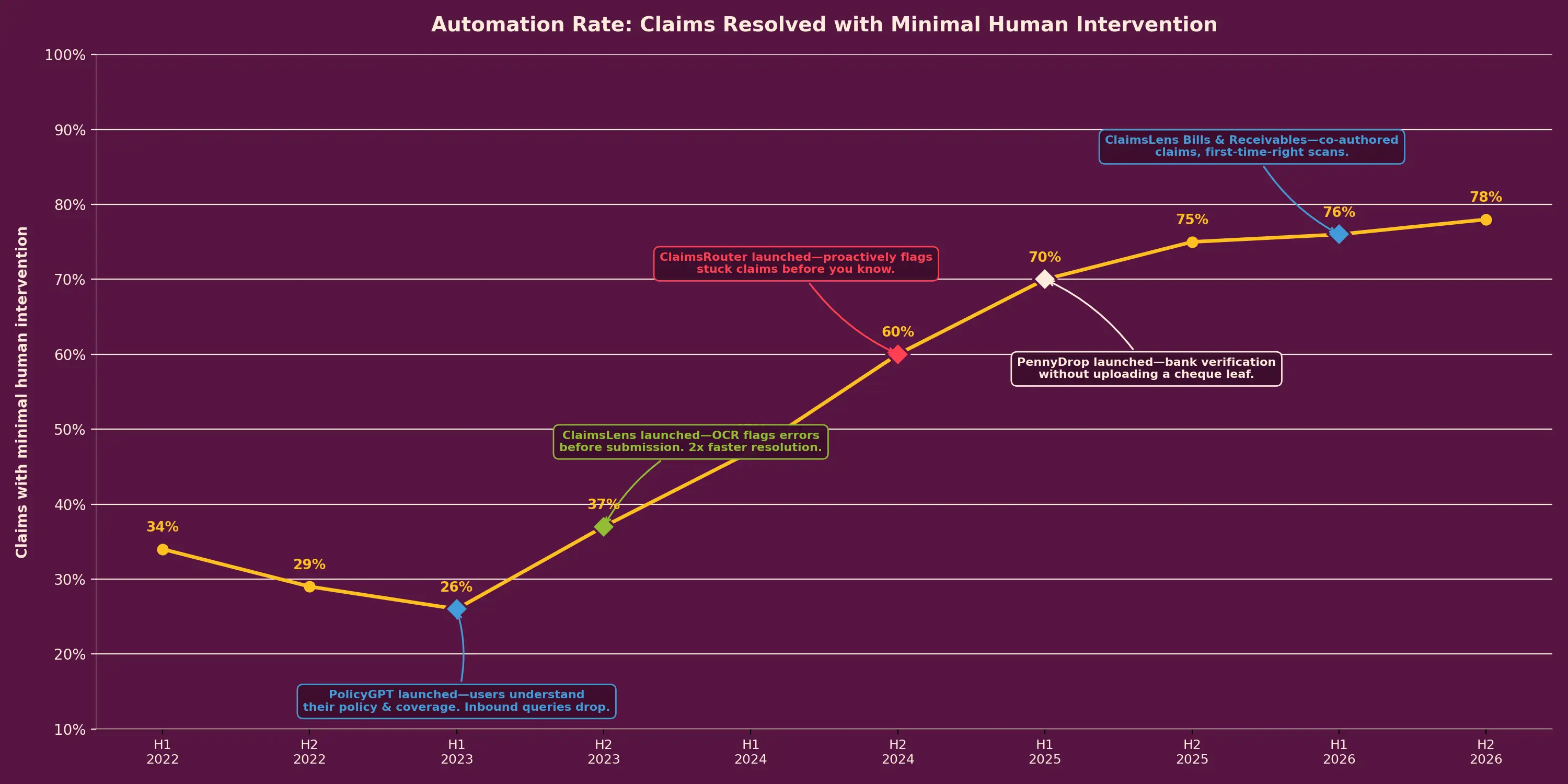
Value
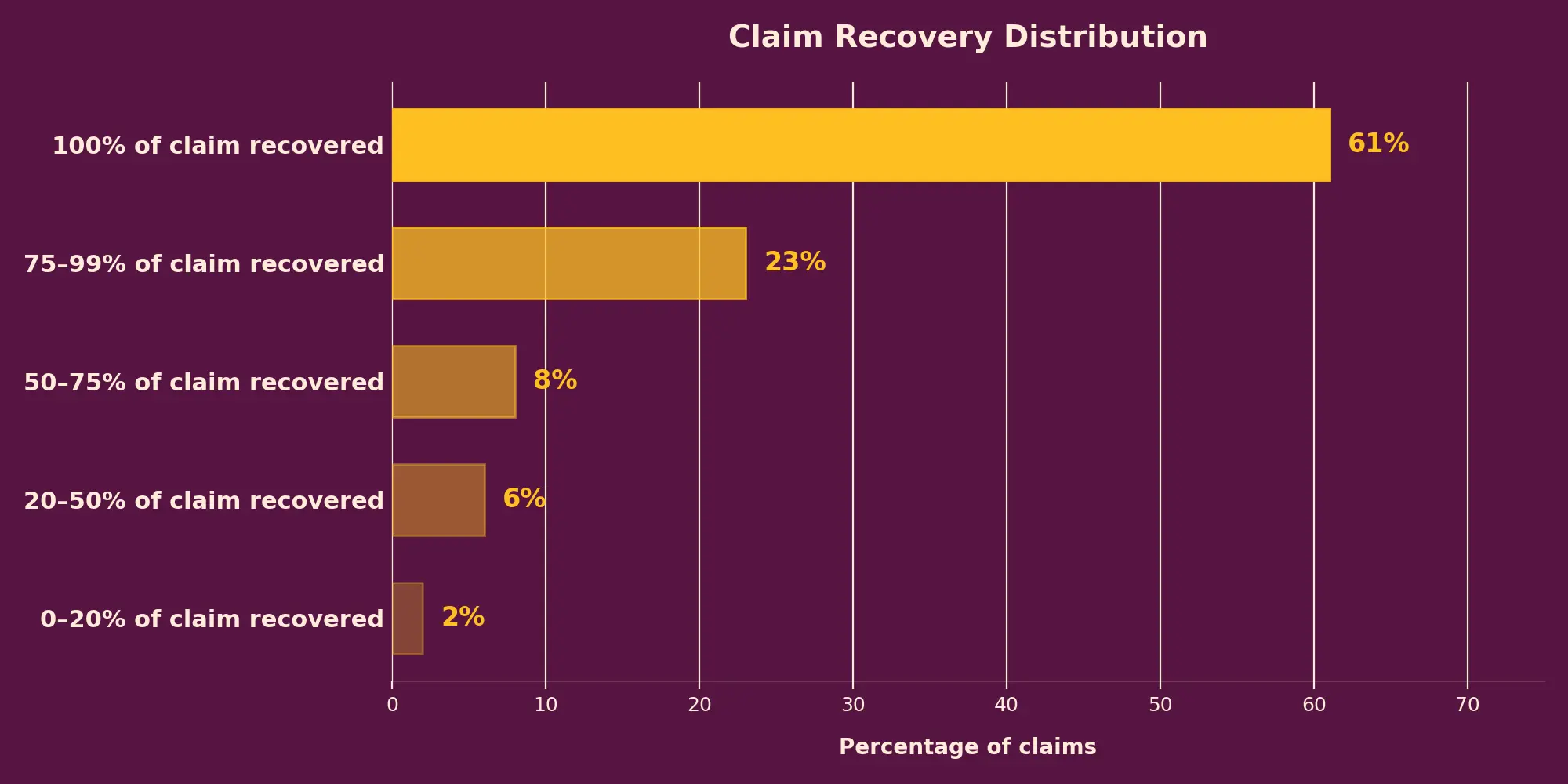
In the unfortunate event of a claim getting rejected by the insurer, we make your case for you. This year alone, we helped recover 100% of the amount in 60% of the cases – translating to INR 10cr of money deposited in our users’ bank accounts.
Ease
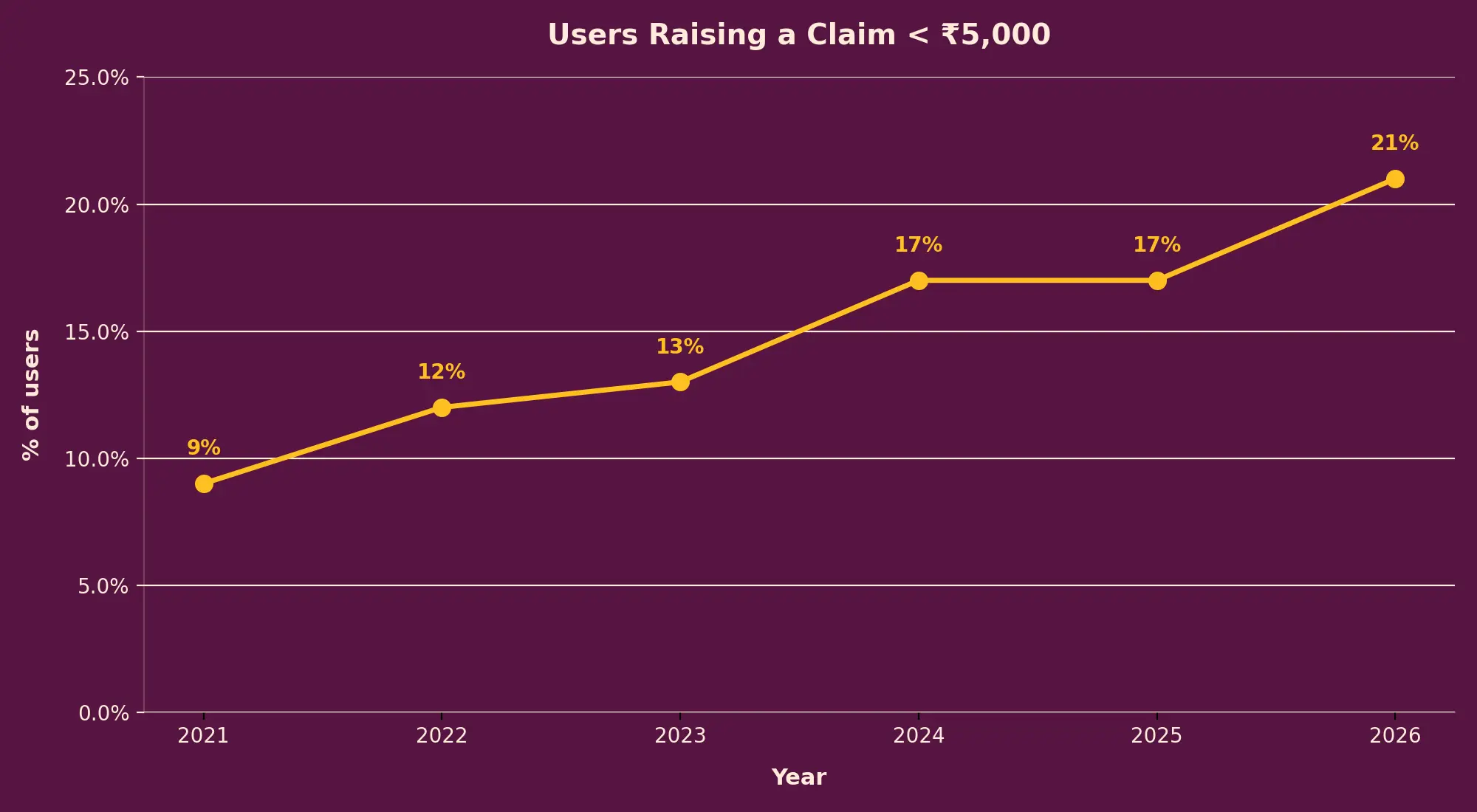
With Plum, you can file a claim in less than 120 seconds on your app. Our user research revealed that users would not raise claims for smaller amounts because the process was so complex that the inconvenience was simply not worth it. A fifth of the claims we process are for amounts under INR 5000. And while most ignore this metric, we see this as a valuable proxy to measure how seamless the claims process is.
Obsessing over claims experience means obsessing over everything that contributes to it. And fixing them bit by bit — the processes, technology, AI interventions, people — it all has to work together.
Zoom out with me for a bit – When you look at claims experience as the best proxy for our success, you realise that something was fundamentally wrong about how group benefits have always been sold. The employee, the person who actually needs to use the product, inherits a policy they did not choose, from a provider they did not pick, for a process they have never been shown.
The claim puts the employee at the heart of it all. You’re solving for a person and consequently for the organization, and not selling a policy and showing up only during renewals.
Doing so also forces us to look at what causes a claim in the first place, urging us to consider the longitudinal nature of health in general for the individual and the organisation. A hospitalisation policy doesn’t capture everything about health – It’s about a consultation for something that does not feel right, a mental health check during a hard quarter, a preventive screening, primary care for their family. The companies that take talent seriously have started thinking this way too.
Companies investing in healthcare in addition to insurance have grown by 120% over the last five years.
Therefore, in a way, prioritizing the claims experience has influenced our growth into a comprehensive employee health company. Personal insurance, primary care, mental wellness, telehealth, flex benefits. None of it came from a strategy document. It all was a natural byproduct of our obsession with the claims experience and the adjacent areas that influence it – today, healthcare contributes to 20% of our total revenue.
This obsession has contributed to our enviable revenue growth, our GWP growth, our NRR and so much more. We're recording our first year of cash flow profitability, which means our conviction stands proven. At scale but also at unit economics levels.
This infinite runway confidence meets product-market-dovetail-fit conviction and tells us that we're ready to take this to the next million people. Through companies that care.
And that is why we’ve raised our Series B of ₹193 crore, to deliver this experience at audacious scale.
Impatience is a wonderful thing to live with sometimes. This capital lets us move at the speed the moment deserves, while raising the bar on the outcomes we deliver.
The assumption in this industry has always been that quality costs time. We have spent six years disproving that. Our claims resolution on cashless is down to minutes from hours. Reimbursement claims get closed in days, not weeks. A telehealth consultation happens on Plum every two minutes. We process over a hundred thousand claims a year. These are not benchmarks we are chasing – but the standard we want to set for insurance and healthcare experiences across the world.
But the more consequential conversation is about what efficiency needs to mean going forward. Work is changing. Teams are getting leaner by design. Managers are being asked to carry more. More decisions, more scope, less support. In that environment, benefits cannot be another thing that requires active management. Health insurance, claims, renewals, endorsements, employee queries, all of it needs to run without creating a burden for the people responsible for running the business.
What an HR team needs from Plum is not a helpdesk. It is a co-pilot. A system that handles the operational weight in the background, surfaces decisions only when a decision is genuinely needed, and otherwise stays completely out of the way. That is the product we are building toward. One where a lean HR team at a five-hundred-person company operates with the same ease and confidence as the best-resourced enterprise in the world.
What’s next
Good businesses last. We intend to be here for a very long time.
Our team will grow. We will go deeper on integrations, security, and the product investment needed to make the full health journey, from prevention through primary to critical care, as well-designed as our claims experience already is. Enterprise-grade is not a label. It is what our customers require, and what we intend to deliver. For all our customers.
To the 500 Plum-bers who chose to build this with us: you are the moat. To our investors, old and new: thank you. To our customers: the trust you place in us with the health of your people is something we think about every day. And to the six hundred thousand employees who have trusted us in their most vulnerable moments: everything we build is for you.
We are ready.
.avif)










.avif)













